![]()
Facilitating the Prescribing Process
When prescribing a therapy covered under a patient’s pharmacy benefit, the provider is typically faced with a series of complex pre-treatments steps and manual workflows. To complete theses tasks he must begin a lengthy process of engagement with various parties to understand how to move forward with therapy.
eACCESSRx offers manufacturers an enterprise solution designed to streamline provider workflows for specialty brands that typically require a Prior Authorization (PA) and fall under the patient’s pharmacy benefit.
Solution Highlights
Help the provider understand and address several key questions:
- What are the patients benefits and how is therapy covered?
- Which manufacturer forms and consents must be completed?
- Is Prior Authorization required and how can I most efficiently address these requirements?
- Which specialty pharmacy can I use to fill the script?
Utilize Technology to Streamline Workflows:
- Combines automated workflows and proprietary transactions (RxeBI and RxePA) to facilitate the prescribing process.
- Includes advanced digital tools to automate workflows (e-signature and e-form completion).
- Delivered as an enterprise solution which includes a provider branded portal with a call center utility.
Achieving Data Transparency Through Real-time Transactions
VirMedica’s ability to leverage its proprietary real-time transactions enables us to deliver on-demand product-specific benefits information and payer requirements to the provider.
These transaction sets include an automated electronic benefits investigation (eBI) and electronic prior authorization (ePA).
Instead of making multiple contacts with the HUB, Payer or PBM, Providers or HUB personnel are able to understand the patient’s benefits and address the payer’s Prior Authorization requirements in moments rather than days.
Using Automation to Streamline Workflows
Today, providers must execute multiple, manual process steps and complete an array of paper forms to access a specialty product. In contrast, with eACCESSRx, manual workflows are simplified and accelerated through automation that leverages the power of Dynamic Data Capture (DDC).
Dynamic Data Capture
With DDC, key data elements are collected and then redeployed to complete required forms as well provide the necessary data inputs to process required pre-treatment steps.
Completing The SRF Triggers Key On-boarding Process
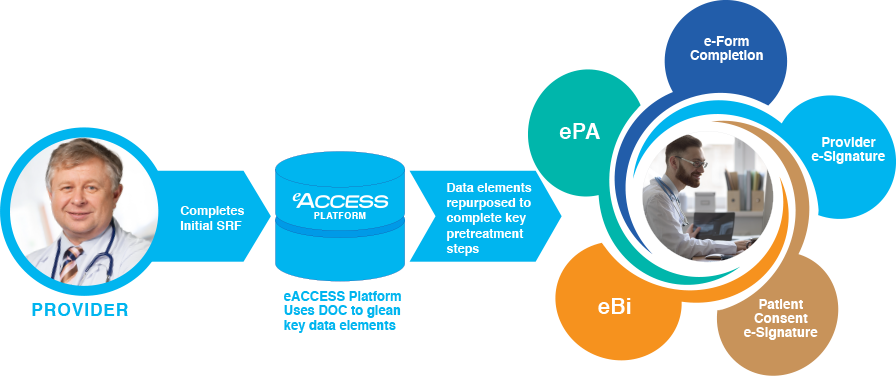
Provider Control & Flexibility
We designed the eACCESSRx solution to ensure that your provider base is not asked to complete any more work than required today to request service.
Providers simply choose how they are going to access your services – completing the Service Request Form (SRF) either online or via fax.
To that end, once the SRF is completed, the provider’s administrative workflow is virtually complete!
Provider Flexibility
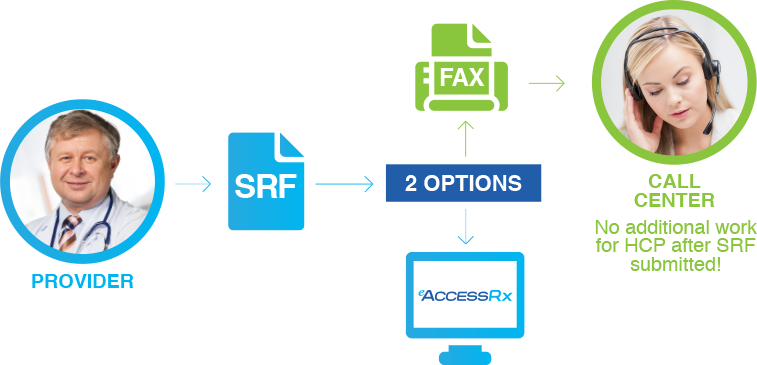
A Prescription for Confidence
Once deployed, eACCESSRx works to create Provider confidence…confidence that once the Service Request Form (SRF) is submitted, all pre-treatment hurdles necessary to write a product-specific script are satisfied and the patient will go onto therapy.
Solution Configuration
Our multifaceted tool is designed to facilitate the most critical workflows of both the provider and/or HUB call center agent including:
- Perform an automated Eligibility and Formulary/Benefit transaction
- Execute an automated Prior Authorization process
- Coordinate and deliver a prospective PA and completed script to the SP
- Deliver real-time information and status updates back to the provider*
*requires the provider portal; not available in standalone call center configuration
As such, eACCESSRx can be used to support provider’s interested in using self-service technology (Provider Portal) or to service doctor’s who prefer to use phone/fax technology (Call Center Portal).

Provider Portal Experience
- Electronic Enrollment Form
- e-signature Enrollment Form
- Initiate and Complete Electronic Eligibility & PA
- Enrollment Form and Eligibility/PA Information forwarded to HUB or SP

Call Center Experience
- eACCESSRx can be made available as a Call Center Portal to enable HUB personnel to deliver a more holistic customer service experience.
- By providing instant access to our tools, call center agents are positioned to efficiently address the Provider’s questions regarding coverage, prior authorization and product access.
- Call Center users have access to – and can view and print – all transaction data that occurs in the Provider Portal.